Regional Network of Excellence in Child Health Care in Ghana
Situation:
The SDG-target for child mortality aims to end preventable deaths of newborns and children under 5 years and to reduce neonatal mortality to 12 deaths per 1,000 live births and under-5 mortality to 25 deaths per 1,000 live births.
Ghana has reduced the mortality rates of neonates (NeonMR), infants (IMR) and children under five years (U5MR) considerably in the last 30 years. The neonatal deaths within the U5MR in 1990 were 33% and 50% in 2019 and the deaths of children under 1 year were 63% of the U5MR in 1990 and over 78% in 2019. The overall reduction of the U5MR is more the result of a reduction in the death of children between 1 and 5 years than of children below 1 year. All efforts to further decrease the U5MR to reach the SDG target should focus on all children holistically – many factors play a role such as nutrition, housing, water, sanitation, environmental issues, road safety, climate change as well as natural disasters etc. – but should pay special attention to health care of neonates and infants.
This focus is supported in Ghana by its health insurance policy. Ghana is one of the few sub-Saharan countries with a functioning National Health Insurance Scheme (NHIS). The majority of people in Ghana are members of the NHIS and pregnant women and newborns up to three months are automatically fully covered. After three months children can be insured for free until 18 years of age, only a small registration fee is demanded. However, child health care has been a neglected area of health care delivery in Ghana for many years which has changed only recently. Most of the hospitals in Ghana do not have a paediatrician. Equally, paediatric specialisation for nurses is hardly existing and has just began within the past few years.
Objectives:
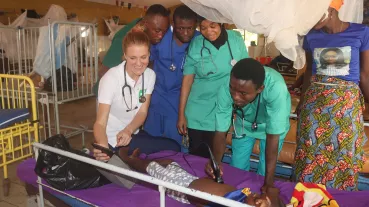
The project aims at reducing neonatal and under-five mortality in the Bono East Region and neighbouring districts in the Bono and Ashanti Regions by establishing a regional network of cooperation between the Holy Family Hospital in Techiman (HFH) and six referring hospitals.
- Standard Operation Procedures (SOPs) of the referral process including the Ambulance Service have been officially put in place by the Holy Family Hospital in Techiman and the six referring hospitals.
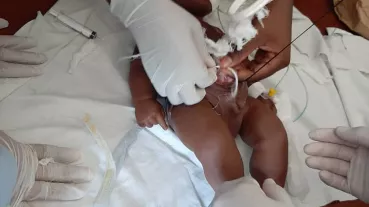
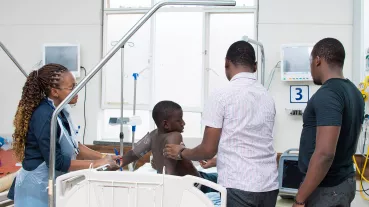
- The staff of the Neonatal Intensive Care Unit (NICU) and the Paediatric Intensive Care Unit (PICU) of the HFH and the staff of paediatric and maternity departments of the six referral hospitals are undergoing a regular training programme and has been assigned permanently to Neonatal Intensive Care Unit (NICU) and the Paediatric Intensive Care Unit (PICU).
- Health education materials to improve positive public attitude to maternal and child health issues are readily available. Talks on local radio programmes take place regularly. Radio features have been produced and are broadcasted.
- Establishing a network structure with a supportive governance structure
- Procurement of essential clinical tools and equipment
- Specialized qualification of paediatric nurses
- Development of Standard Operation Procedures (SOPs) of the referral process and common clinical protocols
- Training of medical and nursing staff including midwives of the paediatric and maternity departments of the Holy Family Hospital in Techiman and the six referring hospitals.
- Public Health education for pregnant women and young mothers.
- Lessons learned and best practices are being documented and fed into the training programmes.
With the development and implementation of SOPs with regard to the referral system efforts right from the beginning will focus on making these procedures routine procedures.
HFH has also a clear general vision to become a training centre, especially with regards to paediatrics. It aims to continue and develop accredited training formats that will be attractive to staff of neighbouring hospitals.
With e-learning methods becoming more and more common and e-conferencing more and more routine practice, cooperation between the HFH as a central facility and the peripheral hospitals will become more and more the order of the day and will even increase instead of decrease after the project support for the network has ended.
The design and implementation are the main responsibility of the management of the paediatric department of the HFH and is thus aligned with the national health strategy. The training programs and standard operating procedures developed in the project serve as a basis and are to be offered to other hospitals and facilities in the future in order to sustainably improve the care of newborns and premature infants in particular.