Anthropomorphes 4D Phantom
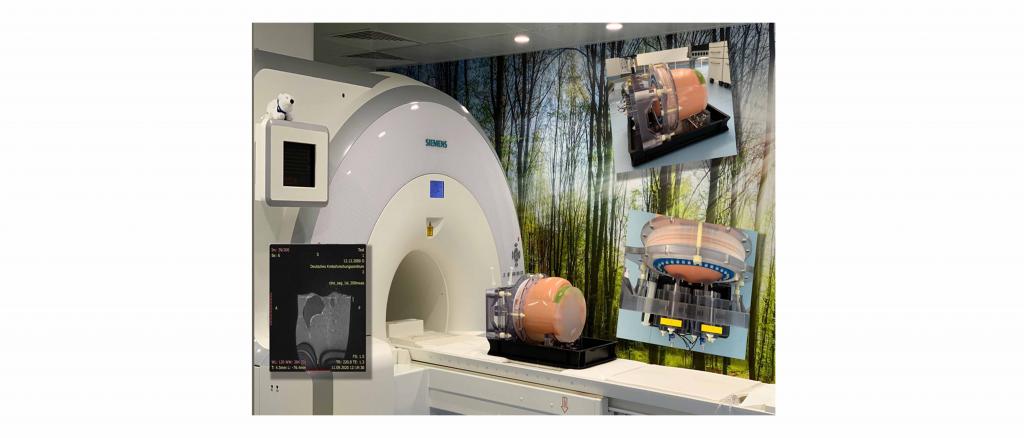
The future of radiation therapy lies in the dynamic adjustment of the target volume during irradiation in real time (image guided radiation therapy). Currently, organ movements are compensated by predicting respiratory curves via gating (interrupting radiation as soon as the target area moves out of the beam). In radiation oncology, adaptive irradiation methods that apply the dose spatially and temporally precisely are becoming increasingly popular. Interferences due to movements, positioning uncertainties and dependence on filled organs (bladder, rectum) are detected in order to optimize the dose distribution in the target volume and to minimize the radiation exposure of the risk structures. This requires continuous adaptation of the precalculated radiation field to the real tumor shape.
Phantoms that reflect the complexity of real patient treatments are used for quality assurance of the individual steps in the entire radiotherapy chain. A phantom that simulates radiological interaction in the body contains several tissue substitutes. Special interaction coefficients are represented by the linear attenuation coefficient and the stopping power, as well as tissue contrasts for imaging, radiation planning, and dosimetry.
The aim of the project is a novel anthropomorphic and dynamic phantom for faster and more efficient quality assurance of adaptive radiotherapy. The phantom represents anatomically realistic organs as well as reproducible movements of the organ composite. It also exhibits human equivalent radiological scattering and absorption properties and realizes the 3-dimensional spatial position change of the target volume. As a result, the dynamics of the entire radiation treatment system can be verified in real time.
The phantom developed by the principal investigators is used for quality assurance of image-guided adaptive radiotherapy and enables an effective end-to-end test of the radiotherapy treatment chain. Its application should enable more precise and tissue-sparing irradiation by minimizing safety margins with fewer side effects and new diseases for the patient. Optimization of irradiation application and greater patient throughput are expected.